|
Common Eye Conditions
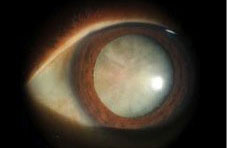
Cataracts
|
A cataract is a clouding of the eye’s normally clear lens, leading to a progressive impairment of vision. It results from the clumping of proteins within the lens, which then distort or block the passage of light as it enters the eye, thus affecting vision. |
Causes
| Ageing | This is the most common factor, as cataract formation is part of the normal ageing process. Most start developing at the age of 40 to 50 but do not affect vision till later in life. The rate of progression or ‘ripening’ also varies between individuals and between both eyes. |
| Eye Injury | |
| Diabetes | |
| Chronic Eye Diseases | eg retinitis pigmentosa, high myopia |
| Medications | eg steroids, radiotherapy |
| Foetal Infections | eg rubella, toxoplasmosis, herpes simplex |
| Ultraviolet Radiation | is a strong risk factor |
| Smoking | is also a postulated risk factor |
Symptoms
- Blurred vision, as if looking through a translucent piece of glass
- Poorer vision even in bright light
- Seeing double or multiple images
- Reduced ability to distinguish colours
- Glare, especially when driving at nights
- Seeing haloes around lights
Diagnosis
It is easily diagnosed and evaluated by an eye doctor, who will then be able to advise on the treatment options.
Prevention
There is no way to prevent the development of age-related cataracts but measures can be put in place to help avoid or slow down their progression in other conditions.
- Good control of blood glucose levels in diabetics
- Limiting use of medications eg steroids, diuretics
- Rubella immunization for women pre-pregnancy
- Monitoring of herpes infections in pregnancy
- Use of sunglasses especially if doing outdoor activities
- Avoid smoking
Treatment
As long as vision remains satisfactory, no treatment is necessary.
When vision starts to deteriorate, your eye doctor may recommend stronger eye glasses or medicated eyedrops as temporary measures.
When poor vision interferes with or disrupts normal daily activities, surgery would then be recommended. It is also not a must to wait till the cataract is ‘ripe’ as advances in microsurgery have made it very safe to remove even those in the early stages.
Currently, the preferred surgical procedure is phacoemulsification. This involves the insertion of an ultrasonic instrument through a small incision in the cornea to break up or emulsify the cataract. The pieces are vacumned out via the same channel, leaving the capsule of the lens behind. An artificial lens implant is then inserted.
Phacoemulsification is usually performed as a day/ambulatory procedure, with a faster recovery period than previous methods of surgery. Complications are uncommon.
Common Eye Conditions
- Age Related Macular Degeneration
- Blepharitis
- Cataracts
- Central Serous Chorioretinopathy
- Contact Lens Problems
- Diabetes and the Eye
- Dry Eyes
- Floaters and Flashes
- Glaucoma
- LASIK Surgery
- Pterygium and Pingueculae
- Refractive Errors
- Retinal Detachment
- Retinal Vascular Disorders
- Uveitis and Ocular Inflammations
- Vision Problems in Children